Transform Your PBM Operations with Cutting-Edge Software

Empowering PBMs and Corporations
Solutions That Transform Pharmacy Benefits
Centric iSolutions delivers innovative PBM software solutions in the United States, helping organizations manage pharmacy benefits with transparency, accuracy, and full control.

Expertise Built Over Decades

Technology that Empowers Ownership
Our custom claims adjudication engine enables PBMs and corporations to fully own and control their core processing system rather than relying on external vendors. This ownership model improves flexibility, reduces long-term costs, and gives organizations greater transparency and efficiency in configuring their benefit programs.

A Network of Industry-Leading Partners
Centric iSolutions collaborates with solution partners who complement our PBM software with features that enhance claims processing, reporting, and integration. This partnership ecosystem ensures clients benefit from a comprehensive, high-end pharmaceutical technology solution built for growth, compliance, and strong operational performance.
Our Story
A Legacy of Innovation in Pharmacy Benefit Technology

Our Services
Technology That Transforms Pharmacy Benefit Management
Centric iSolutions provides advanced pharmaceutical technology solutions in the United States, offering PBMs and corporations access to a flexible, scalable, and transparent technology ecosystem. Our services help organizations manage claims, process pharmaceutical data, and optimize benefit structures with greater control. Every solution is built on real-time processing, secure data integration, and a modern PBM technology platform that adapts to evolving business needs.
Claims Processing Software
Our Claims Processing Software in the United States provides PBMs with a reliable and accurate platform for an end-to-end pharmacy claims management system. Built to support complex benefit structures, the system processes pharmacy claims in real time and ensures every transaction is handled with precision
- Real-time claim validation
- Automated rule-based adjudication
- High-accuracy processing
- Scalable for PBMs of all sizes
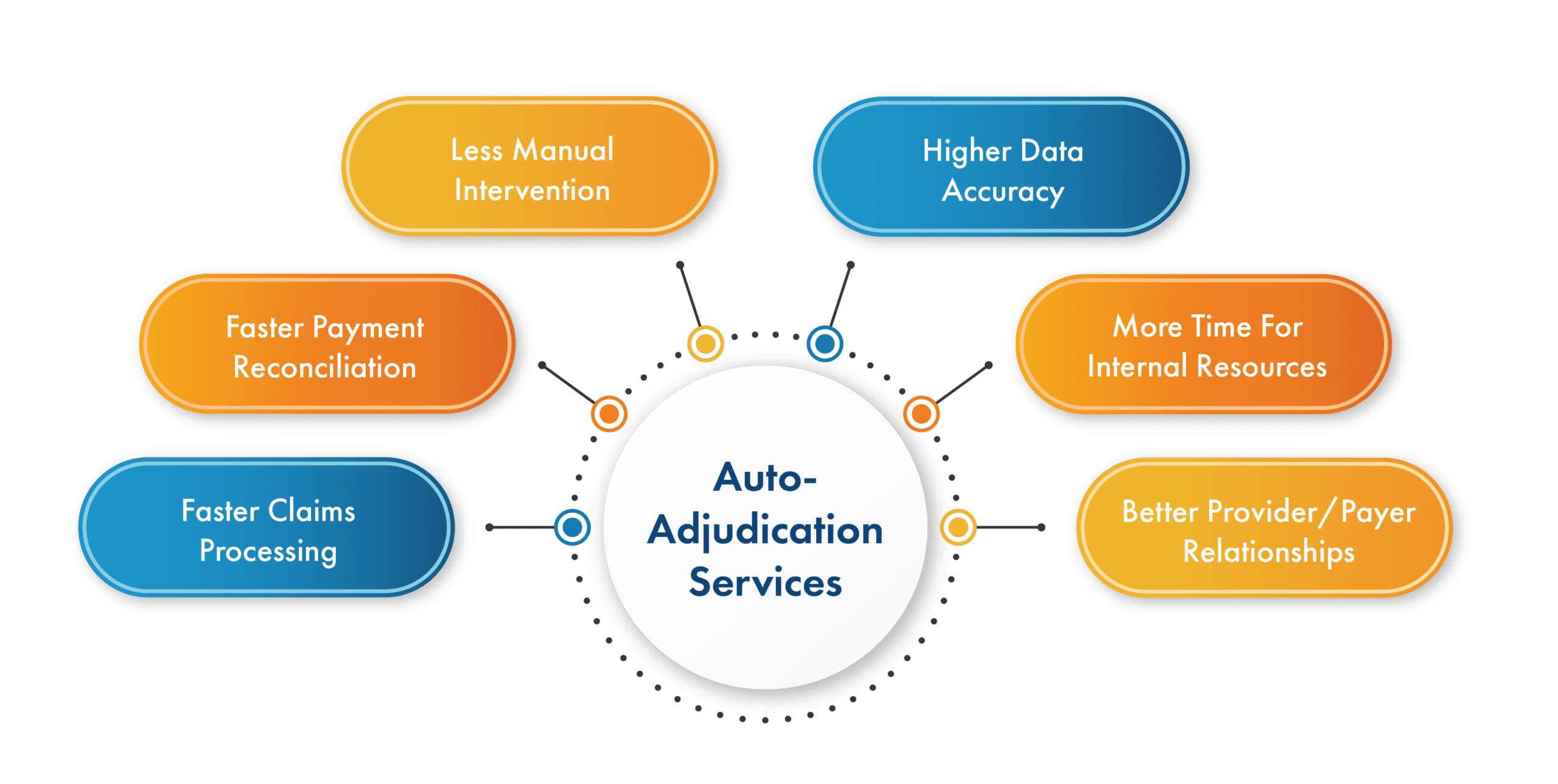
Custom Claims Adjudication Engine
- Full system ownership
- Custom rule configuration
- Real-time data integration
- High-volume performance stability
PBM Technology Platform
- Integrated partner ecosystem
- Advanced analytics and reporting
- Real-time operational visibility
- Built for PBMs and corporations

Take Control with Advanced Claims Processing Technology
Get in Touch
We Are Ready to Support Your Pharmacy Benefit Technology Needs
If you have questions about our claims processing software, want to explore our custom adjudication engine, or wish to discuss PBM technology for your organization, we are here to assist. Reach out to us for product guidance, partnership discussions, or tailored technology consultations.
